What are Fluoroscopy-Guided Injections?
Fluoroscopy is a real-time imaging technique that allows healthcare providers to visualize the internal structures of the body. In the context of joint injections, fluoroscopy guides the needle’s placement, ensuring accurate and targeted delivery of the medication.
Fluoroscopy enhances accuracy so well that the Joint Relief Institute offers a 100% Accuracy Guarantee.
Hyaluronic Acid Injection success rate is greatly improved by the Fluoroscopy-Guided injection process. When considering knee or shoulder gel injections for pain relief, be sure to seek out a provider that uses the process.
The Benefits of Fluoroscopy-Guided Injections
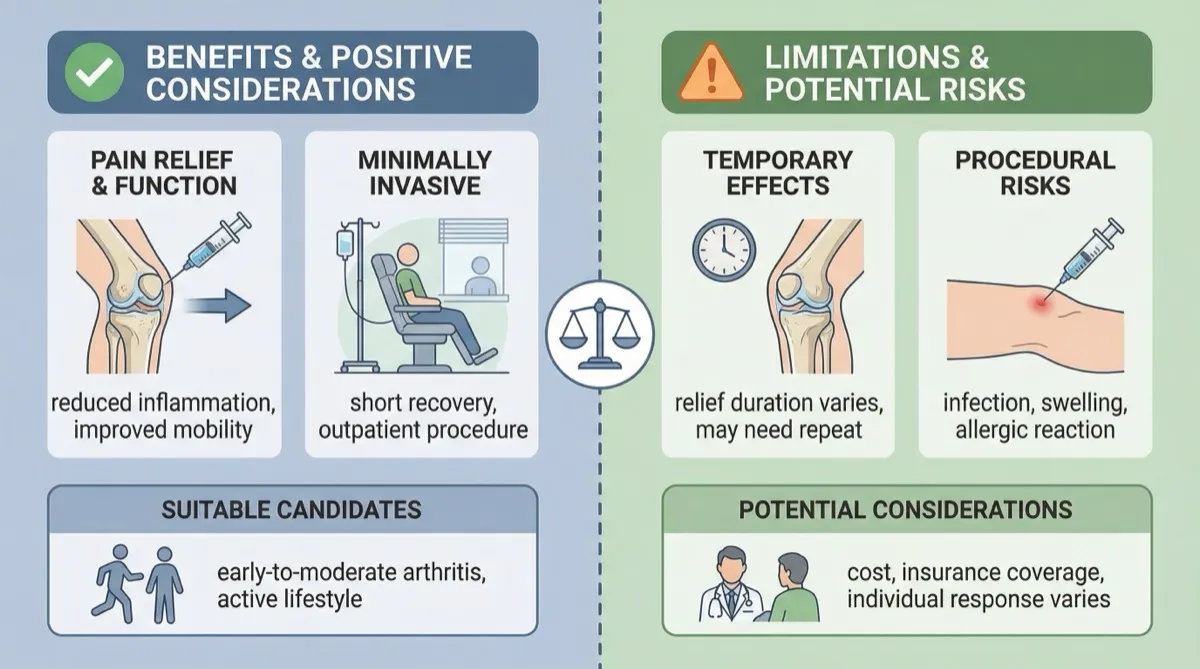
- Enhanced Accuracy: Fluoroscopy provides real-time visualization, minimizing the risk of misplacement and ensuring that the medication reaches the intended target.
- Reduced Complications: Accurate needle placement reduces the risk of side effects, such as pain, swelling, and infection.
- Improved Patient Outcomes: Precise delivery of medication can lead to more effective pain relief, increased joint mobility, and a longer duration of benefit.
The Importance of Precision in Gel Injections
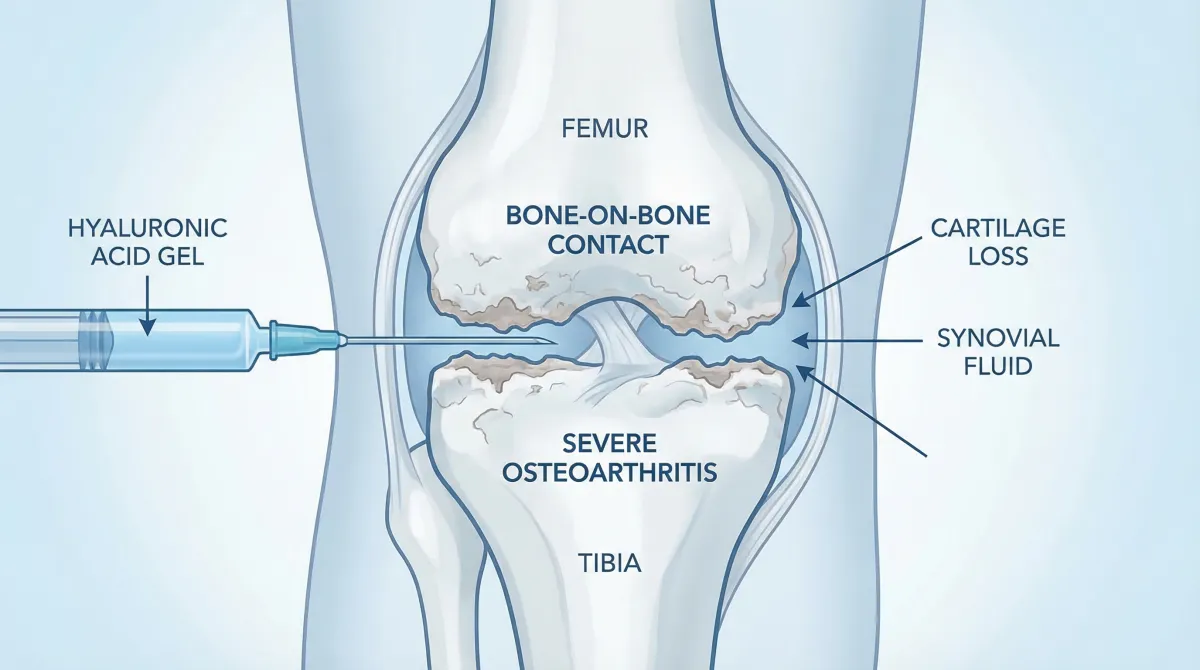
Hyaluronic acid injections have become a popular non-surgical treatment for osteoarthritis. However, the effectiveness of these injections depends largely on precise needle placement within the joint. This is where fluoroscopy-guided injections are greatly beneficial.
Fluoroscopy-Guided Injections: A Study in Effectiveness
A study published in the Journal of Medical Case Reports (PMCID: PMC4190177) examined the effectiveness of fluoroscopy-guided hyaluronic acid injections for hip and knee osteoarthritis. The study found that patients who received fluoroscopy-guided injections experienced significant pain relief and improved joint function compared to those who received traditional blind injections.
Furthermore, according to another study, non-guided injections missed the joint up to 30% of the time. When injections miss, the treatment is completely ineffective, making fluoroscopy essential for the success of injections.
Does the Joint Relief Institute Use Fluoroscopy-Guided Injections?
Yes. At The Joint Relief Institute, we prioritize patient care and utilize fluoroscopy to ensure the highest level of accuracy and effectiveness in our gel injection procedures. By using this advanced technology, we can help patients achieve optimal results and experience significant relief from joint pain.
Contact Us Today
To learn more about knee gel injections, their costs, and insurance coverage, please contact us:
- Chicago Office: (708) 722-7514
- Edina (Minneapolis) Office: (952) 214-4278
Fluoroscopy-guided injections represent a significant advancement in the field of joint pain management. By ensuring precise needle placement, this technique can improve patient outcomes and reduce the risk of complications. If you’re considering hyaluronic acid injections, consider seeking a provider who utilizes fluoroscopy to maximize the benefits of your treatment.